Dr. Nadine Burke Harris – TED Talk on Adverse Childhood Experiences
 Watch on YouTube
Watch on YouTube
The first video I ever found on trauma and health. It was eye-opening — and genuinely infuriating — to realise this talk was already nearly a decade old, and the ACE Study behind it was from 1997. Almost thirty years of evidence. I was only just finding out.
If you only do one thing on this site — make it watching this video.
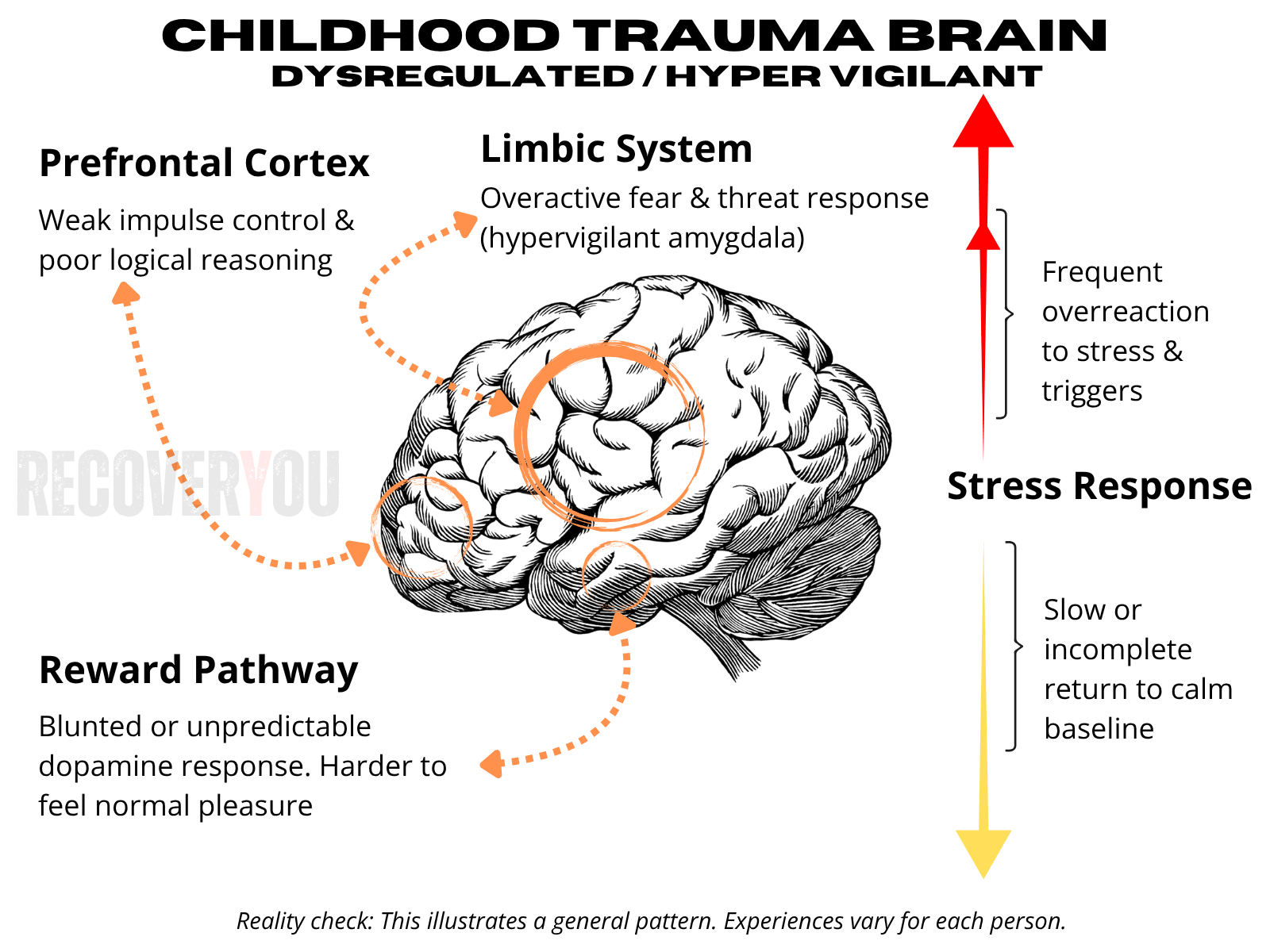
When I first watched this talk by Dr. Nadine Burke Harris, it felt like someone had finally put language to everything I had lived. She laid out exactly how early adversity reshapes biology, alters brain development, and sets the trajectory for lifelong health outcomes. This single video became the epicentre of everything on this site — not just my understanding of addiction, but the first time I started to understand myself.
And then came the frustration. The talk was already almost ten years old when I found it. The research behind it — the original ACE Study — was from the late 1990s. Nearly thirty years of evidence sitting in plain sight, and nobody in medicine, education, or treatment had ever once handed it to me. Not once. I had to stumble onto it alone, in my thirties, while trying to figure out why my life looked the way it did.
That frustration didn't go away. It became the fuel behind everything I've built here — a refusal to let this information stay buried in academic journals and TED playlists while people who needed it most kept asking the same unanswered questions I did. If it took me this long to find it, how many others are still searching?
This talk remains one of the most powerful entry points for understanding how trauma embeds itself in the body — and why awareness, as unglamorous as it sounds, is often the first real act of recovery.