What Toxic Stress Does
Stress is supposed to come and go. The body spikes, then resets. Toxic stress is what happens when the reset never comes, when the stress systems stay locked on.
- SAM Axis (Sympatho-Adreno-Medullary // Adrenaline): Fires instantly, preparing the body for fight or flight. Heart races, breath quickens, muscles tense.
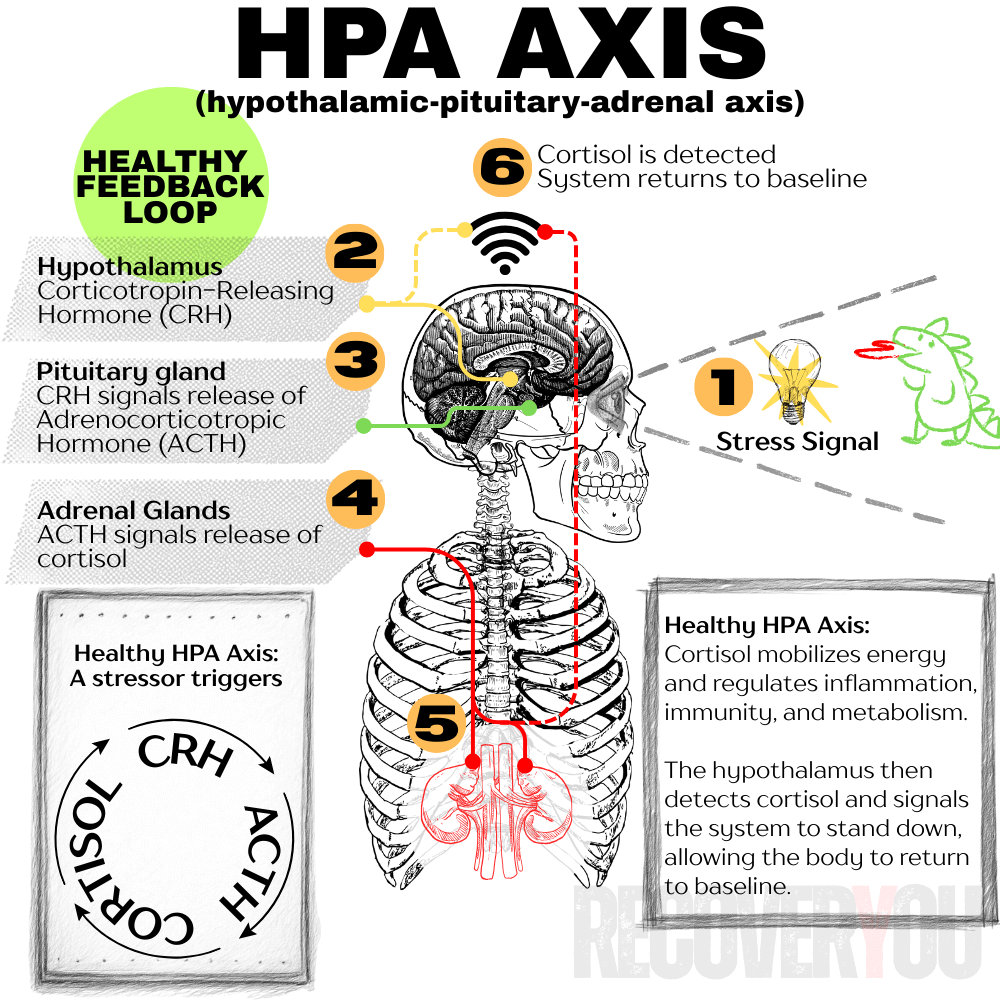
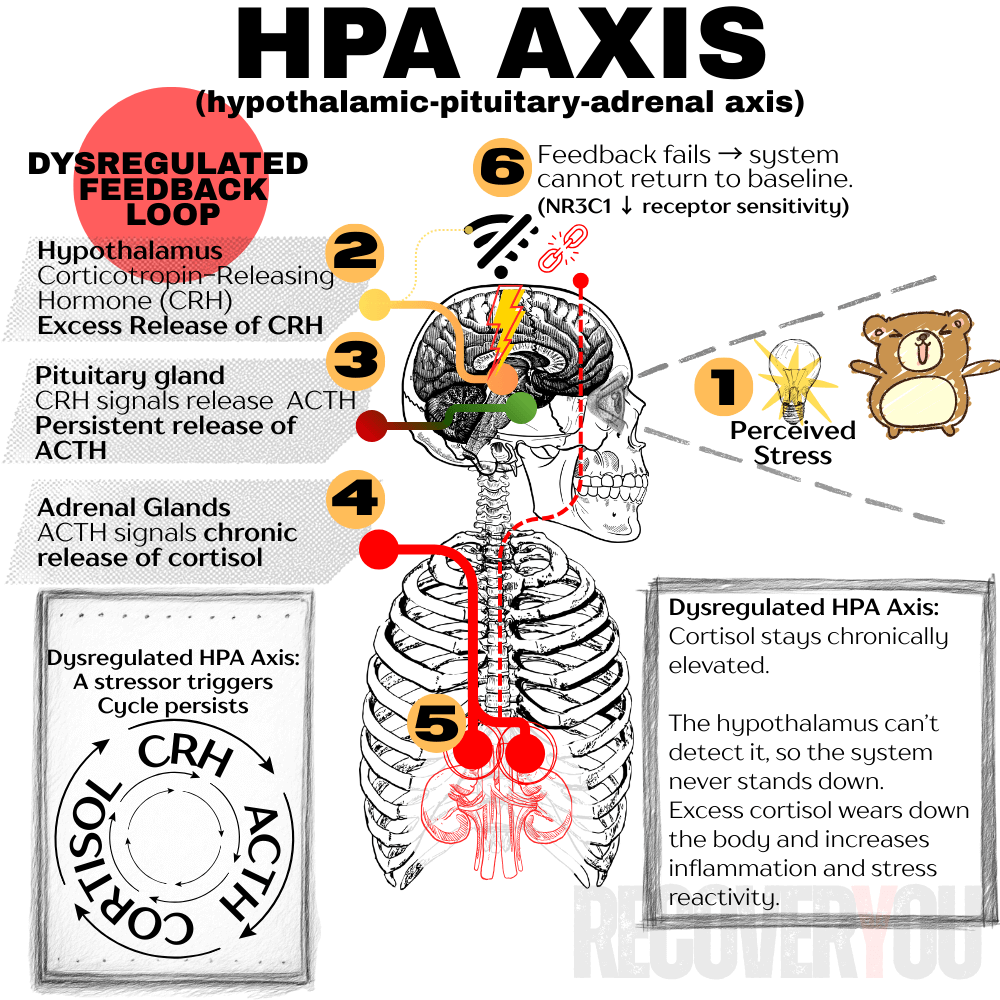
- HPA Axis (Hypothalamic-Pituitary-Adrenal // Cortisol): Kicks in slower, but lasts longer. In short bursts, it helps. In chronic doses, it reshapes the brain.
Key brain regions affected:
- Prefrontal Cortex: The brakes. Responsible for logic and impulse control. Trauma stunts its growth.
- Amygdala: The accelerator. The brain's threat-detection system. Trauma strengthens its wiring and keeps it on high alert.
- Hippocampus: Memory and context. It helps the brain separate what's happening now from what belongs to the past, and signals when the alarm is safe to shut off. Chronic cortisol exposure shrinks it, weakening both memory and the brain's ability to stand down.
These systems don't operate in isolation. When the hippocampus can no longer place experience in time, the stress response stays active as if the threat is still happening, even when it isn't.
This imbalance is called allostatic load: the wear and tear of being stuck in survival mode. Instead of growth, the brain prioritizes vigilance. The ANS is central here: the sympathetic branch stays overactive, the parasympathetic branch underfunctions, and the system that should bring relief never fully engages.
Toxic stress doesn't just shape emotions. It wears down the body. Research links it to heart disease, diabetes, autoimmune conditions, and shortened lifespan. This is allostatic load made visible.
In children, the line between healthy stress and toxic stress comes down to one thing: a reliable buffer. A caring, attentive adult who helps regulate the child's nervous system and turn off the alarm. Meeting new people, starting school, falling off a bike, these are normal developmental stresses the brain can learn from, when safety and comfort follow. Without that buffer, or worse, when the caregiver is the source of fear, the child has no way to reset. Safety never arrives. The body stays on high alert. The brain wires for survival instead of growth.
Even one consistent, supportive adult can change this trajectory. Safety doesn't erase trauma. But it reshapes how the brain organizes itself around it.